Clinic for maternal-fetal medicine
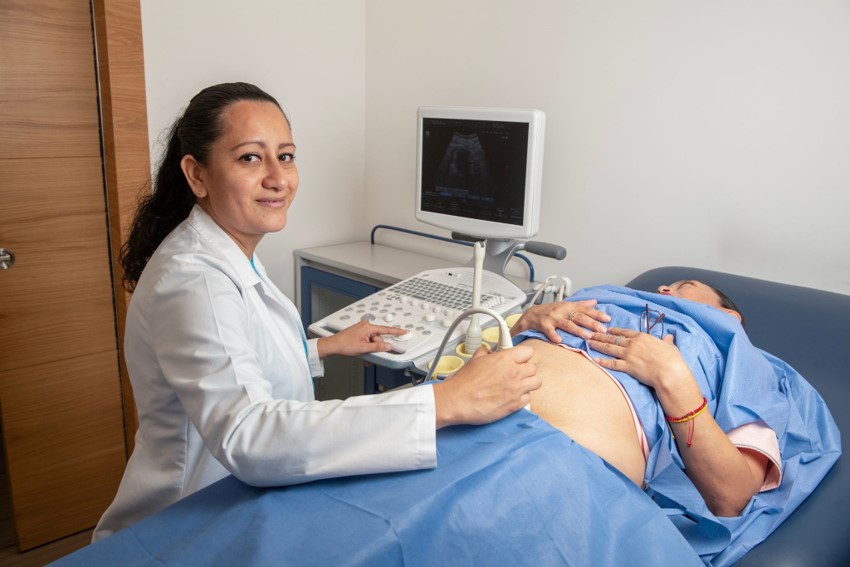
Pregnancy is an beautiful and fascinating event, that ideally, progresses without any complications until the birth. However, some pregnancies are considered high risk pregnancies, due to conditions that affect both the mother’s and the baby’s health. A high-risk pregnancy occurs when there are factors prior or during the pregnancy that increase the risk of perinatal complications.
Some risk factors can be treated in order to reduce their negative effects, while others can’t be modified, they require rigorous monitoring. This approach allows much more control, all oriented towards a safer, more positive result for the mother and for the baby.
Frequently Asked Questions
• How can I know if my pregnancy is a high-risk pregnancy?
The risk must be assessed ideally before conception. Preconception risk factors can be identified in previous gynecologic consultations, which allows the couple to work in order to reach optimal health conditions before the pregnancy. In the consultations the doctor will take a thorough medical history, also some routine tests and if the doctor considers it necessary, some special test will be made, like a level 2 ultrasound. At the end, the OB/GYN specialist will determine if the pregnancy could be high-risk or not.
• Which are the most common risk factors?
1. Socio-demographics: If the patient is 19 years old or younger, or older than 35 years old, if there was bad prenatal control, if the patient has given birth more than 5 times, her weight is under 50 kg, and/or if the patient has bad habits.
2. Surgical or medical diseases: Diabetes, hypertension, epilepsy, thyroid diseases, kidney conditions, asthma, lupus, arthritis, and hematologic conditions.
3. Obstetric factors: If the patient has had any abortions, experienced fetal deaths, underweight newborns, premature deliveries, uterine malformations, and thrombosis.
4. Pregnancy complications: Fetal growth restriction (FGR), threatened preterm labor (TPL), preterm premature rupture of membranes (PPROM), hemorrhages, gestational diabetes, and recurrent infections.
5. History of complications during labor: Urgency caesarean section, vaginal tears, postpartum incontinence, and birth asphyxia.
What are the measures taken in a Control Plan?
After the evaluation, the specialist will give a detailed explanation of a specific control plan and some recommendations to achieve a pregnancy with the least probability of complications. This risk factors assessment can only be made by an OB/GYN specialist.
